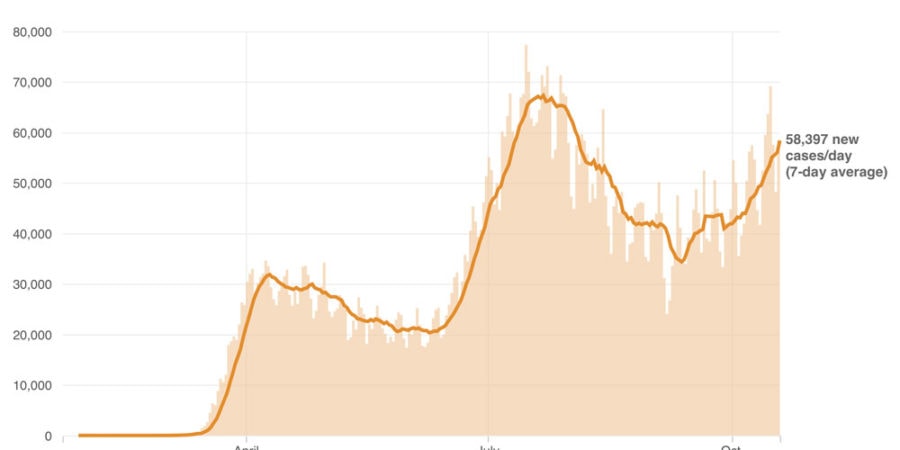
New Cases of Coronavirus (COVID-19) Surge to Highest Level Since July
A surge of new coronavirus cases in the U.S. has the potential to surpass the growth of COVID cases seen in July during the “summer surge”. The seven-day average for new infections is now more than 58,000 per day, an increase of 30% from two weeks ago. While 29 states and territories have reported a rising number of cases, this third surge is predominantly affecting the Midwest and Rocky Mountain regions. Largely spared earlier in the pandemic, more than a third of all new cases in the U.S. last week were reported from states and rural communities in this region.
Health experts predicted the coronavirus would likely gain traction in the fall, when more people spend time indoors, when respiratory viruses are typically seen, and students are usually returning to schools and college campuses. The steep rise in COVID cases and how early it is happening however was not anticipated. According to Dr. Peter Hotez, dean for the National School of Tropical Medicine at Baylor College of Medicine, “It’s happening at a rate that is even faster than I might have expected. I predict then we’ll soon start seeing the number of deaths go up.”
Dr. Hotez isn’t alone. Given the current trajectory of the pandemic, models are forecasting the surge to continue and eventually exceed 100,000 new cases a day, including a death toll of 170,000 individuals in the coming months.
According to Dr. Amesh Adalja, a senior scholar at the Johns Hopkins University Center for Health Security, “the biggest issue is still the fact that many of these states don’t have the capacity to test, trace and isolate.”
“We are caught in the middle of a COVID storm,” stated North Dakota’s Governor Doug Burgum. New infection rates in North and South Dakota exceed all other states, including what Arizona experienced during the summer surge.
Of particular concern is the decline in rural areas to emergency care, largely the result of too few patients to stay afloat financially during the pandemic. Rural communities also have higher rates of underlying conditions and behaviors that make their populations more susceptible to COVID. These include smoking, high blood pressure, obesity, and diabetes. COVID related deaths lag a month or so behind case counts. According to the COVID Tracking Project, there were 39,320 people in 40-plus states with the disease in hospitals as of Tuesday, October 20 – the highest number seen since August 22, and eight consecutive daily increase.
Hospitalizations in Wisconsin more than doubled in the past two weeks, requiring the state to create a field hospital to make room for the growing number of infected patients. Mark Kaufman, the chief medical officer for the Wisconsin Hospital Association stated all seven of the state’s health care emergency readiness regions are seeing “record and near-record numbers of hospitalized COVID patients.”
Other states including California, Illinois, Montana, Wyoming, Utah, New Mexico, Florida, Texas, Tennessee and Mississippi are also experiencing a spike.
Since the outbreak began, the U.S. has reported more than 8.27 million COVID infections – more than a fifth of the world’s nearly 40.8 million cases. In the U.S. more than 221,000 people have died of the coronavirus. The U.S. currently ranks 11th among 168 nations for the highest number of deaths, as tracked by Johns Hopkins. While the overall death rate for those hospitalized has declined, possibly due to doctors and nurses knowing how to better treat the disease it causes, this third surge of infections could push states and especially communities in rural areas beyond hospital capacity – even in states that have previously succeeded in limiting the pandemic’s spread.
For more information on how BLU-MED hospital surge tents, patient screening shelters, negative pressure isolation systems, or field hospitals, can quickly expand your hospitals capacity, contact us today using the following:
| Phone: | 888-680-7181 (Toll Free) |
| 425-739-2795 (US) | |
| Email: | inforeq@blu-med.com |
| Web: | Complete our online contact form. |